New lease on life for heart valve patients
Minimally-invasive TAVR procedure at OSF HealthCare can mean better recovery
At 94 years old, every day counts for Jim Bier.
The Champaign, Illinois, resident, U.S. Army veteran, and retired map-maker is able to manage things like visiting the store and strolling his backyard gardens – a space resembling the University of Illinois Japan House gardens, which Bier designed. It all comes with less chest pain and easier breathing thanks to a minimally-invasive heart procedure offered at OSF HealthCare.
“I’ve been at home, exercising, building up my legs, and I don't have the difficulties breathing like I did before all this happened back in the garden days,” Bier says. “And so I would say I'm in very good shape at this point.”
Bier pauses and adds with a chuckle, “From my waist up. I still have to work on my legs.”
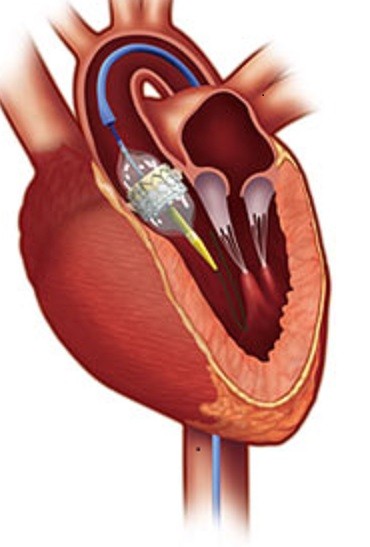
Approved by the U.S. Food and Drug Administration in 2011, transcatheter aortic valve replacement, or TAVR for short, deals with a thickened aortic valve in the heart that can’t fully open. This reduces blood flow and could mean symptoms like chest pain, shortness of breath, fainting, and fatigue.
Tariq Enezate, MD, a cardiologist at OSF HealthCare Cardiovascular Institute in Urbana, Illinois, explains that the TAVR procedure begins with making a small cut near the patient’s groin. The doctor then inserts a small catheter – “smaller than my little finger,” Dr. Enezate notes – and guides it up to the heart to insert a new valve. This is opposed to the more invasive open-heart surgery, which can lead to a longer and more painful recovery for the patient. Minimally-invasive surgeries like TAVR also avoid the need to stop the patient’s heart.
“Those patients are old. They have a lot of diseases. So, many of them, they are not good candidate for surgery. And the surgery team might think they might not be in good shape and strong enough to handle the stress of open heart surgery,” says Dr. Enezate of potential TAVR patients. “In those situations, TAVR is actually lifesaving.”
For Bier, the lifesaving series of events began on Christmas Eve of 2021. By then, Bier had been dealing with heart problems for nearly a decade and had used a blood thinner after open heart surgery didn’t yield the best results. But a visit to the emergency department that day turned into a week-long stay and the question: What more needed to be done? Eventually, Bier says doctors told him about one last surgery that was needed – “the big one,” as Bier puts it. He needed a new heart valve.
An avid reader, Bier researched the TAVR procedure to allay his concerns.
“I’m a person who goes with the flow,” Bier says. “You talk to any of the nurses who've dealt with me at the hospital. They're saying all the time, ‘Go with the flow.’ That's what I kept telling them all the time. And in that way I'm pretty optimistic about it.”
Still, Dr. Enezate recognizes that even minimally-invasive heart surgery may cause stress. He says the patient’s care team – everyone from the cardiologist to the anesthesia team – meets with the patient and their family several times before the procedure.
After TAVR patients go home, Dr. Enezate explains, they eventually will enter cardiac rehabilitation to rebuild the strength needed to do the everyday activities they love. Other appointments with a provider and medications like a blood thinner are also typical.

“We have a big team of doctors, nurses, nurse practitioners, therapists, social workers, and so many people. Take care of the patient, take care of their family, answer their questions, get the tests, the procedures that they need. And after the procedure, we are on top of things.”
“We have a big team of doctors, nurses, nurse practitioners, therapists, social workers, and so many people,” Dr. Enezate says. “Take care of the patient, take care of their family, answer their questions, get the tests, the procedures that they need. And after the procedure, we are on top of things.”
At OSF HealthCare Heart of Mary Medical Center in Urbana, where TAVR recently launched, that team includes Dr. Enezate, Ashraf Al-Dadah, MD, Alaa Ujayli, MD, and Kelli Lamaster, the cardiac program coordinator. Each of them undertook years of schooling and training to be able to successfully oversee operations like TAVR.
“If you asked a cardiologist 10, 20 years ago and you tell them a patient with valve replacement can go home next day, they would think that you're crazy,” says Dr. Enezate. “But now, it is reality.”
Visit the OSF HealthCare TAVR website for more information and to find a provider near you.
Interview clips - Jim Bier
Interview clips - Dr. Tariq Enezate
B-Roll
Previous TAVR stories from the OSF HealthCare Newsroom
Mick Jagger Recovering After TAVR Procedure - April 5, 2019
Forging the Path – TAVR for Congenital Heart - December 10, 2021
New Innovations are the Heartbeat of TAVR - November 3, 2022


